My Cancer Diagnosis
“If you or someone you love is facing cancer, this new video series offers a powerful, real-life look at the journey—from the shock of diagnosis to treatment, recovery, and everything in between. Through honest storytelling and firsthand experience, each episode shares the challenges, decisions, and emotions that come with navigating cancer, while also highlighting moments of strength, resilience, and hope. This series is created to inform, support, and connect with others who may be walking a similar path. Whether you’re searching for answers, encouragement, or simply want to feel less alone, these videos are here to remind you that there is a community that understands and cares. From where I stand, whether I win this fight or loose it, I know my Savior Jesus Christ has my back until the very end”
Medical Disclaimer
The information provided on this page, “Cancer Diagnosis,” along with video content shared on my YouTube channel (Warriors Spirit 1961), is based on my personal cancer journey.
It is shared to inform, support, and inspire others who may be facing similar challenges.
While I openly share my experiences, insights, and what I’ve learned along the way, this content is not medical advice, diagnosis, or treatment.
I am not a doctor or licensed healthcare professional. Every cancer journey is different, and what I’ve experienced may not apply to you. Always speak with your physician, oncologist, or qualified healthcare provider before making any decisions about your health or treatment.
While I do my best to share accurate and honest information, I cannot guarantee completeness or accuracy. By using this website and watching my videos, you agree that any reliance on this content is at your own risk, and I am not responsible for any outcomes related to its use.
If you are experiencing a medical emergency, please seek immediate professional medical care.
What to Expect Upon Receiving a Cancer Diagnosis
Executive Summary
Receiving a cancer diagnosis can be shocking and overwhelming to say the least! However, knowing the next steps helps. This guide covers immediate actions (medical, emotional, practical), understanding your diagnosis (tests, staging, prognosis), treatment decisions (options, second opinions, trials), managing symptoms/side effects, emotional support, family communication, financial and legal considerations, coordinating care and advance directives, and trusted resources. The information is organized for easy reading, with bullet checklists and diagrams for clarity. Authoritative sources (NCI, ACS, CDC, etc.) back each section. Use this as a roadmap to navigate your journey.
Purpose and Target Audience
This content is intended for newly diagnosed cancer patients and their families (unspecified cancer type). It uses clear, empathetic language. It assumes a Western healthcare context (primarily US/Canada) where patients might have health insurance or social programs.
It covers adults of any age, but includes advice for talking to children. The advice should be adapted to local healthcare systems and legal rules. (Details like exact benefits or resources will vary by region.)

Immediate Steps After Diagnosis (Medical, Emotional, Practical)
After your diagnosis, focus on gathering information and support. Ask your doctor clearly: “What type of cancer is it and where is it located?” and “What tests have confirmed this?”. Get copies of biopsy or imaging reports for reference. Use a notebook to write down key facts (diagnosis, stage, doctors’ names) and bring it to appointments.
- Schedule follow-up tests/consults: If more imaging or blood tests are needed before treatment, arrange them promptly.
- Bring a support person: Take a family member or friend to appointments. They can help you remember information and provide emotional support.
- Ask questions: Write down questions as they come to you. Good questions include: “What is my cancer stage and what does it mean?” or “What is the goal of treatment (cure, control, comfort)?”.
- Tell loved ones: When you feel ready, share the news with close family/friends. Explain the basics (type of cancer and planned treatment) in simple terms. Let them know how they can help (meals, rides, child care) and how you’re feeling. Giving them specific ways to help can ease your burden.
- Self-care and emotions: A cancer diagnosis often brings shock, fear, or anger (all normal. Take a deep breath. Allow yourself time to process. Rest and eat when you can. If you feel overwhelmed or anxious, ask to talk with a counselor or use patient support hotlines (see resources below).
flowchart LR A[Symptoms or Screening] --> B[Visit Primary Doctor] B --> C{Diagnostic Tests} C -->|Imaging (CT/MRI)| D C -->|Biopsy| E D & E --> F[Cancer Diagnosis Confirmed] F --> G[Discuss Type, Stage, Treatment Goals] G --> H{Treatment Options} H --> I[Surgery] H --> J[Chemotherapy / Immunotherapy] H --> K[Radiation Therapy] H --> L[Targeted / Hormonal Therapy] I & J & K & L --> M[Begin Treatment] M --> N[Follow-Up Care] N --> O[Survivorship / Ongoing Support] Figure: Typical journey from first symptoms to diagnosis to treatment and follow-up.
Understanding Your Diagnosis (Tests, Staging, Prognosis)
Get details: Ask exactly what type of cancer you have (e.g. “breast cancer” vs. “sarcoma”) and where. Ask which tests (MRI, CT scans, blood work, etc.) confirmed it. The most definitive test is usually a biopsy (examining tissue). The biopsy report (pathology) will name the exact cancer subtype. Ask your doctor to explain any big terms. Keep all test results in a folder.
- Staging: Cancer is given a stage (often I–IV) describing how far it has spread. For example, Stage I usually means small/localized, and Stage IV means spread to distant organs. Stage guides treatment decisions. Ask, “What is my cancer stage, and what does that mean for treatment?”.
- Prognosis: This is the likely outcome. It depends on cancer type, stage, and overall health. Ask your doctor what the expected outcomes are in your case. Remember, statistics (like 5-year survival) are just general guides. Everyone is different.
- Additional tests: Ensure any needed biomarker or genetic tests are done (some treatments depend on specific mutations or receptors). Ask, “Do I need more tests before deciding on treatment?”.
- Second opinion on diagnosis: If there’s any doubt, it’s fine to have the diagnosis double-checked by another specialist (many patients do this). A second pathologist or cancer center review can confirm the findings.
Treatment Decision Process (Options, Second Opinions, Clinical Trials)
Your treatment will depend on the cancer’s type, stage, and your health. It may include surgery, chemotherapy, radiation therapy, targeted/hormonal therapies, immunotherapy, or a combination. Make sure your care team explains each option clearly.
- Discuss treatment goals: Ask your oncologist, “What is the goal of this treatment? Can it cure the cancer, control it, or is it palliative (symptom-focused)?”. Understanding the goal helps you align it with your priorities.
- Personal priorities: Consider your life situation (work, family, fertility, finances). For example, if having children is important, ask about fertility preservation before treatment. If travel or cost is an issue, discuss that too. ACS advises weighing cultural/spiritual beliefs, costs, and personal responsibilities when deciding.
- Risks and benefits: For each option, list pros and cons. Ask about likely side effects and how they can be managed. The table below compares key factors to consider.
- Second opinion: It’s okay to consult another cancer specialist (surgery, medical, or radiation oncologist). Getting another opinion is common and can confirm the plan or offer new ideas. Your doctor can refer you or you can contact a major cancer center directly.
- Clinical trials: Ask if there are trials for new treatments that might fit you. Clinical trials often test new drugs or approaches. Participation is voluntary; talk with your doctor or call services (like ACS’s trial-matching) to see if a trial could be an option.
| Factor | What to Consider |
|---|---|
| Cancer type & stage | Certain treatments only work for specific types/stages. More advanced stages often need multiple therapies |
| Your overall health | Your age and other medical conditions affect what you can handle (strong chemo, major surgery require good health). Discuss any concerns (heart disease, diabetes, etc.) with your team. |
| Goal of treatment | Is the plan curative (to cure) or palliative (to control symptoms)? Aiming to cure might mean intensive therapy; if not, a gentler approach may be chosen. |
| Side effects | All treatments have side effects. Weigh how much side effect burden you can tolerate. For example, chemo may cause fatigue, nausea, hair loss, while radiation side effects depend on the body area. |
| Personal values/timeline | What matters most to you—length of life vs. quality of life? Do you want to minimize time spent in hospital? Will you be away from family? Factor these into the decision. |
| Logistics & cost | How far will you need to travel for treatment? Can your insurance cover these treatments? Will you miss work? These practical issues can influence choices. |
| Alternative or integrative approaches | Discuss any complementary therapies (acupuncture, yoga, meditation) with your doctor—they can help with symptom relief if used safely. Treat *any alternative therapy with caution; approaches not proven effective can be harmful*. |
Your care team should make sure you understand each treatment’s purpose and process before you start. Do not feel rushed—take time to decide. After this discussion, you will start treatment with confidence in the plan.
Cancer Symptom and Side-Effect Management
Cancer treatments often cause side effects. It’s important to report symptoms early; many are treatable. For example, pain control is a vital part of cancer care. If you have pain, tell your doctor – they will find ways (medications, nerve blocks, therapy) to ease it.
Some Common Chemotherapy Issue:
- Nausea/vomiting: Common with chemo. Doctors can prescribe anti-nausea drugs. Eating small meals, ginger tea, or relaxation may also help.
- Fatigue: Extreme tiredness is frequent. Rest when needed but also try gentle exercise (a short walk) to boost energy. Your team can check for anemia or thyroid issues if fatigue is severe.
- Infection risk: Some treatments lower immunity. Avoid crowds when possible, wash hands often, and contact your doctor immediately if you get a fever.
- Hair loss and skin changes: Chemo can cause hair loss (scalp, brows). It’s temporary; covering your head (hat, scarf) is an option. Skin or nail changes are usually manageable with creams or gentle care.
- Long-term effects: Ask about late side effects (e.g. lymphedema swelling after lymph node removal). Your doctor will plan follow-up screenings to catch any recurrence early.
- Palliative care: Regardless of treatment intent, palliative care specialists can help manage symptoms (pain, breathing, nausea) and improve quality of life. They work alongside your oncology team.
Risks from Surgery:
- Excessive nerve pain around the surgical incision with possible permanent nerve damage.
- Risk of Infection.
- Dry mouth.
- Jaw pain.
- Pain in the incision region. This of course depends upon the type of surgery and where the surgery was.
- These are common effects and can effect everyone slightly different.
NOTE: The surgery image displays a neck dissection commonly used to remove cancerous lymph nodes.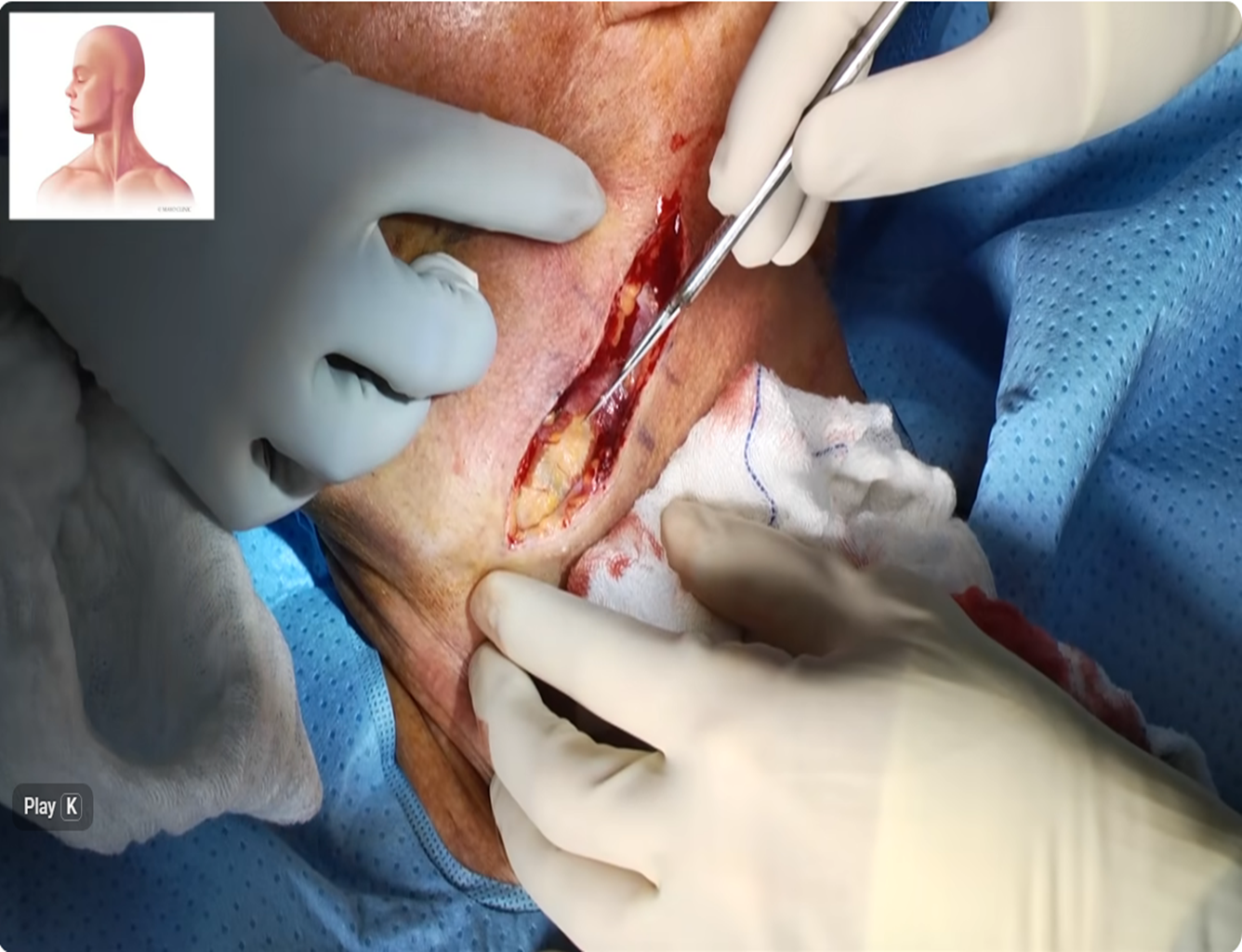
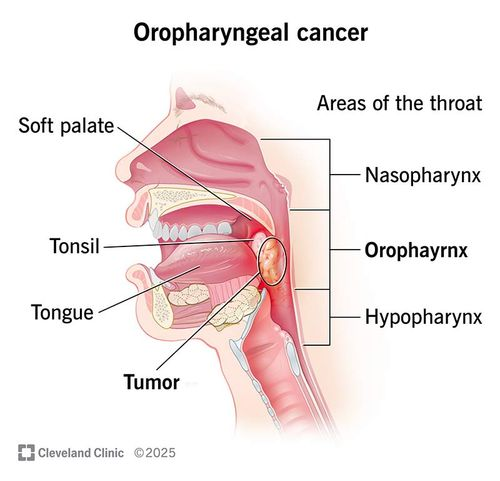
- Oropharyngeal cancer is a type of head and neck cancer that forms in the middle part of the throat (oropharynx), specifically affecting the base of the tongue, tonsils, soft palate, and the side and back walls of the throat.
- High Risk: If left untreated for too long, the cancer often spreads to the surrounding Lymph Nodes requiring “Neck Dissection” to remove the effected Nodes.
Radiation Therapy
Radiation therapy uses high-energy X-rays or particles to damage cancer cell DNA, killing cells or stopping their growth. At high doses it can cure cancer, shrink tumors, or slow tumor growth. Doctors often use it before surgery (to shrink a tumor) or after surgery (to kill any remaining cells), and it can relieve symptoms (e.g. pain) by reducing tumors. External beam radiation is given by aiming a machine at the tumor; advanced forms (IMRT, SBRT, proton therapy) precisely shape the beam. Brachytherapy (radioactive seeds placed inside or near the tumor) and systemic radiopharmaceuticals (radioactive drugs) are also used. Treatments are planned by a simulation session (imaging and custom molds) and delivered in daily small doses over a few weeks, followed by follow-up visits. 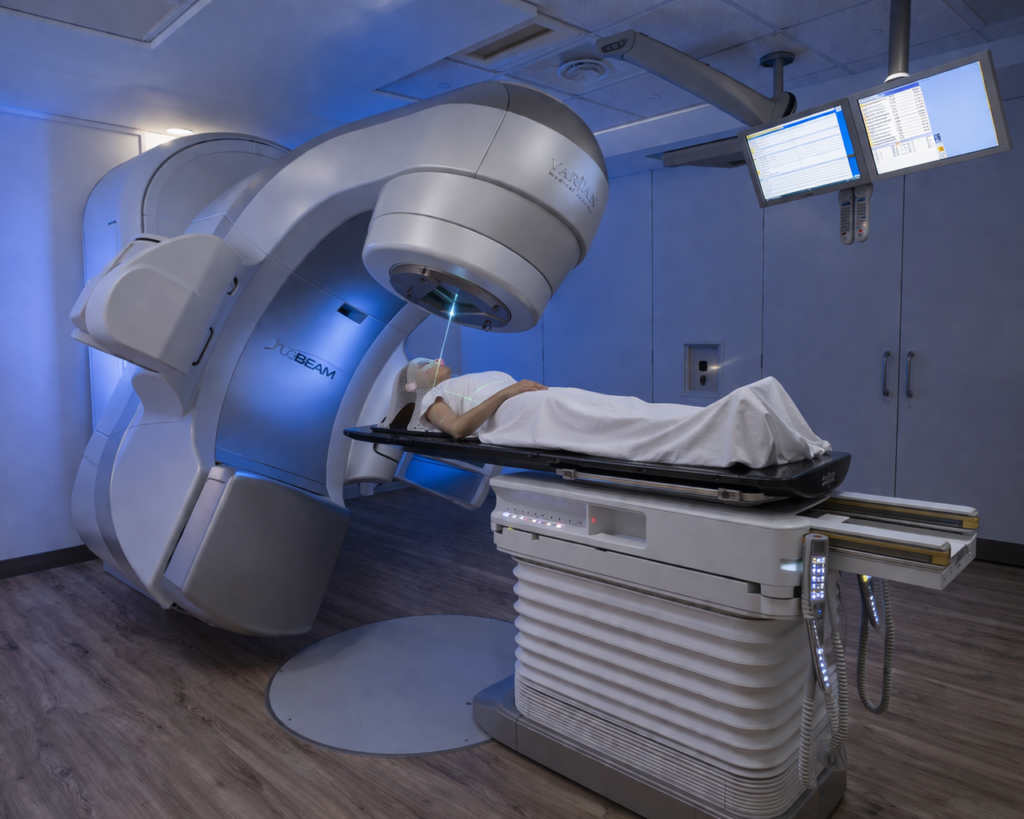
Side effects occur because normal cells near the tumor can be affected. Common short-term side effects (during or shortly after therapy) include skin redness, fatigue, mouth or throat sores, nausea or diarrhea (depending on where radiation is given). Late effects (months to years later) can include scarring of normal tissue or, rarely, a second cancer. Risks rise with higher doses, concurrent chemotherapy, or factors like smoking. Your care team will monitor side effects and manage them with medications (pain relievers, anti-nausea drugs), topical creams or mouthwashes, nutritional support and rehabilitation as needed. Patients should ask their radiation team what side effects to expect and how to address them, as well as questions about protective measures (e.g. skin care tips or breathing exercises) during treatment.
Sources: Trusted cancer resources (NCI, ACS, etc.) explain that radiation damages DNA in cancer cells and is used for cure, control, or palliation. Side effect information is based on NCI’s radiation therapy fact sheets
Radiation Mask
A radiotherapy mask is a custom-molded thermoplastic device that holds a patient’s head, neck, or shoulders perfectly still during radiation treatment. Made by warming a plastic mesh and shaping it to the patient’s face, it hardens within minutes and ensures highly precise radiation delivery while protecting healthy tissue.
Key points:
- Purpose: Keeps the body immobile for accurate, consistent treatment—especially for brain, head, and neck cancers.
- Creation: A warm, flexible mesh is placed over the face and molded to fit exactly.
- Use: The mask is secured to the treatment table to maintain the same position each session.
- Comfort & Safety: Snug but breathable; patients can still communicate with staff.
- Skin Care: Reused across sessions; may leave temporary pressure marks.

Managing discomfort:
- Communication: Talk to your care team about anxiety or claustrophobia.
- Preparation: Viewing the mask beforehand and completing dental work can help reduce stress and ensure proper fit.
- Reducing Anxiety: While not shown in this image, eye & mouth slots can be cut out of the mask which makes it more tollerable.
Emotional and Mental Health Support
Feeling anxious, scared, or depressed is normal after a cancer diagnosis. It’s important to address these feelings:
- Express your feelings: Talk about fears or frustrations with someone you trust (spouse, friend, clergy). You can also keep a journal or use online forums to share anonymously.
- Professional help: Ask your doctor for a referral to a counselor or psychologist experienced with cancer patients. Many centers offer free support groups or one-on-one counseling. These services can teach coping skills and provide comfort.
- Support groups: Joining a support group (in person or online) connects you with people facing similar challenges. CancerCare and the ACS host groups for various cancers. Sharing experiences often brings relief.
- Self-care: Make time for relaxing activities (reading, music, gentle walks). Try mindfulness or breathing exercises to reduce stress. Maintain routines as much as possible, and prioritize adequate nutrition and sleep.
- Stay hopeful: Focus on day-to-day goals (finishing a treatment week, planning a small outing). Celebrate small milestones (like completing chemo cycles). These can boost morale.
Family and Communication Guidance
Cancer affects the whole family. Being open and planning ahead makes things easier:
- Talking to family and friends: Share your diagnosis when you feel ready. Explain clearly: *“I have [type] cancer in [location]. My doctors plan to [treatment plan].”* Encourage your loved ones to ask questions. Reassure them you will work with your doctors at every step.
- Ongoing Communication: With Your Oncologist and their Team.
- Accept help: Family and friends often want to help but don’t know how. It’s okay to tell them exactly what you need (meals, rides, help at home).
- Small tasks (like walking the dog or dropping off groceries) can be big helps.
- Talking to children: Use age-appropriate language. For young kids, you might say “Mom has a sickness called cancer. The doctor will give me medicine to help me get better.” Give simple answers and reassure them it’s not their fault. Stick to routine for them and involve them gently (e.g. let them pick a toy to bring to the doctor).
- Couples and partners: Cancer can change roles in a marriage or partnership. Talk openly with your partner about fears or changes in intimacy. Consider couples counseling if stress is high. Many couples find that staying connected (hugging, hand-holding) provides comfort.
Financial, Insurance, Leave, and Legal Rights
Managing money and work while getting treatment can be challenging. Here are key points:
- Insurance help: Contact a social worker or financial counselor at your hospital. They can help you understand coverage and co-pays. In the U.S., the American Cancer Society has programs to answer insurance questions. Keep copies of all bills and explanations of benefits.
- Leave from work: In the U.S., eligible employees can take up to 12 weeks of unpaid leave under the Family and Medical Leave Act (FMLA) for a serious illness like cancer. This protects your job and continues health coverage during the leave. In Canada, you may qualify for up to 26 weeks of EI sickness benefits, and provinces like BC and Ontario provide job-protected sick leave up to ~27 weeks.
- Disability benefits: Ask about short-term disability insurance (if your employer offers it), or federal disability programs, which may pay part of your salary during treatment.
- Legal protections: Laws prohibit discrimination based on illness. The ADA (Americans with Disabilities Act) in the U.S. and Canadian human rights laws require employers to accommodate serious illness. If you face job issues, agencies like the U.S. Department of Labor provide guidance on your rights.
- Financial aid programs: Many charities and foundations help with cancer-related costs (travel, child care, home care). For example, Patient Advocate Foundation and HealthWell Foundation in the U.S., or local cancer societies, offer grants. Ask your social worker for specific programs.
Care Coordination and Advance Planning
Cancer care often involves many doctors (surgeon, medical oncologist, radiation oncologist, etc.). Staying organized is key:
- Treatment summary: Before leaving the clinic, request a written summary of your diagnosis and treatments received. This “treatment summary” should list your cancer type, stage, surgeries, medications (with doses and dates), and any side effects noted. Keep this in your personal file and bring it to all appointments.
- Follow-up plan: Ask when and how often you will have follow-up visits and tests after treatment ends. Knowing your follow-up schedule helps you plan and prevents missed tests.
- Point person: Choose one person (or yourself) to act as a care coordinator: keeping track of appointments, managing paperwork, and communicating changes to the rest of the family. This avoids confusion among multiple family members.
- Advance directives: It may feel early, but discuss and complete advance care planning (appointing a healthcare proxy and writing a living will) if you haven’t already. These legal documents specify what treatments you do or do not want if you are unable to decide later. Your doctor or social worker can help you fill out the forms.
- Palliative care: Remember that you can request palliative care at any stage. This team focuses on relieving symptoms (pain, nausea, shortness of breath) and supporting emotional/spiritual needs alongside curative treatments.
flowchart LR Patient -->|Sees| PrimaryCare[Primary Care Doctor] PrimaryCare -->|Refers| Oncology[Oncology Team] Oncology --> Surgeon[Cancer Surgeon] Oncology --> Radiation[Radiation Oncologist] Oncology --> Chemo[Medical Oncologist (Chemo)] Oncology --> Support[Palliative/Social Worker] Support -->|Coordinates| Resources[Support Services] Figure: Example care team flowchart. Your oncologist coordinates with surgeons, radiologists, counselors, and support staff.
Trusted Resources and Support Organizations
Professional and community organizations can help you find information and support:
- National Cancer Institute (NCI): Authoritative cancer info (cancer.gov) and a helpline (1-800-4-CANCER) for questions.
- American Cancer Society (ACS): Patient guides and a 24/7 helpline (1-800-227-2345). ACS offers support groups and practical programs (rides, lodging, wigs).
- CancerCare: A nonprofit offering free counseling, support groups, and financial assistance. Their website has guides on coping, nutrition, and advance directives.
- Local cancer societies: In Canada, the Canadian Cancer Society (cancer.ca) provides support and info. In the UK, Cancer Research UK (cancerresearchuk.org) has patient information. Many countries have similar organizations.
- Support groups: Search for groups by cancer type or age (e.g. young adult). Online forums (ACS Cancer Survivors Network, Inspire, etc.) let you connect with other patients.
- Financial/legal help: Organizations like the Patient Advocate Foundation (US) offer co-pay assistance and case management. Legal aid societies or cancer patient advocates can advise on employment rights and disability benefits.
Checklist
- Get a clear statement of your diagnosis (type and stage) and a written treatment plan.
- Note all doctor names and contacts. Keep a binder of your medical records.
- Ask all your questions (see sections above for examples). Don’t leave an appointment uncertain.
- Arrange transportation and someone to accompany you if needed.
- Report any new symptoms or severe side effects to your doctor immediately.
- Apply for workplace leave or benefits if you need time off (FMLA/EI). Document your treatments.
- Lean on loved ones: delegate tasks and ask for help with daily chores.
- Consider advance directives (healthcare proxy, living will).
- Explore financial aid programs early (ask a social worker for resources).
Glossary
- Biopsy: A test where a small piece of tissue is taken for examination to diagnose cancer.
- Pathology report: A lab report from your biopsy, describing the exact cancer type and characteristics.
- Oncologist: A doctor who treats cancer (e.g. medical oncologist for drugs, surgical oncologist for surgery, radiation oncologist for radiotherapy).
- Staging: A way to describe how far cancer has spread. Often stages I (early) to IV (advanced).
- Prognosis: The likely course and outcome of the disease. It is based on experience but not a certainty.
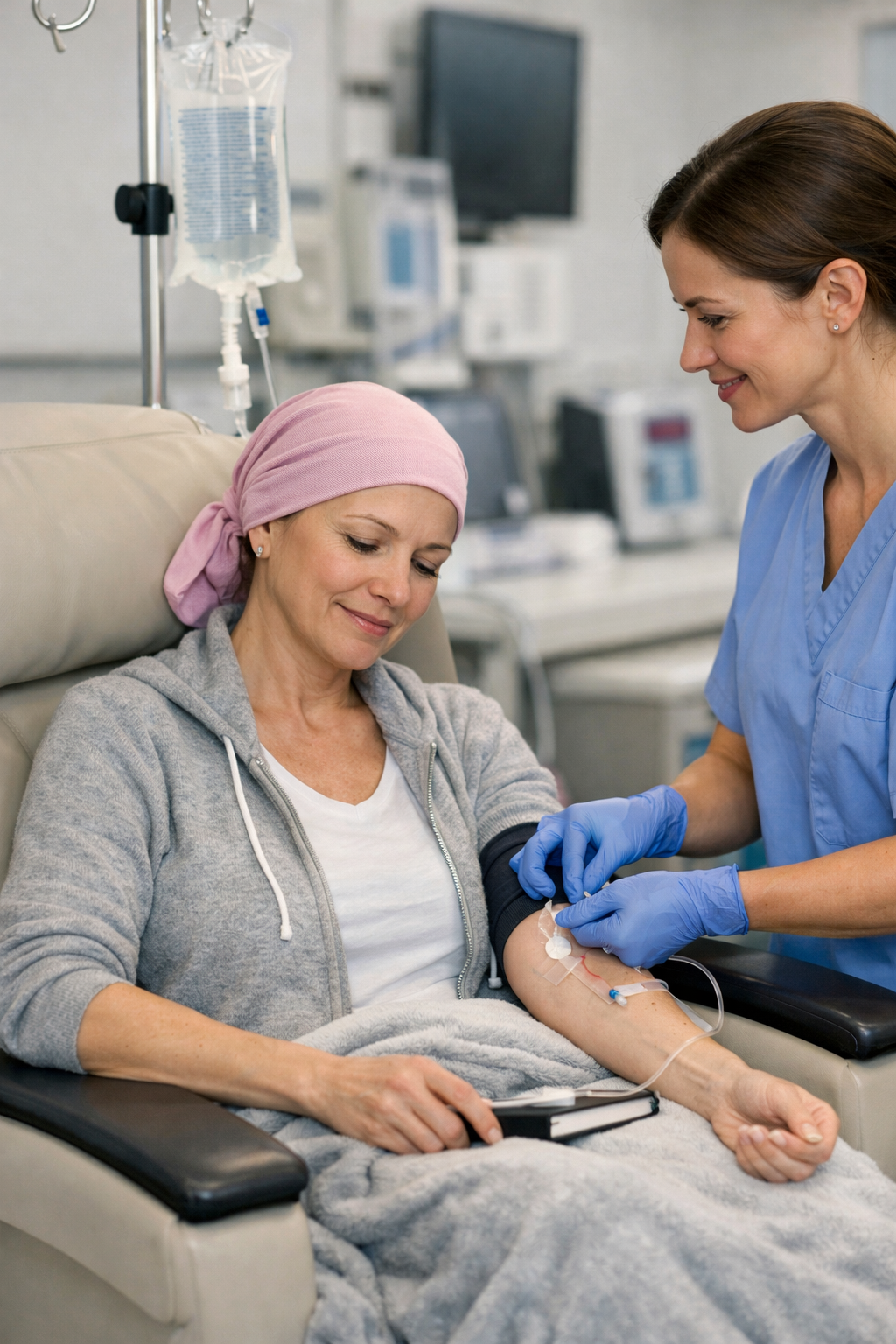
- Chemotherapy: Cancer treatment with strong anti-cancer drugs. Usually intravenous or pill. Common side effects: nausea, hair loss, fatigue.
- Radiation Therapy: Treatment using high-energy rays (like X-rays) to kill cancer cells. Side effects depend on the area treated (e.g. skin changes, tiredness).
- Targeted Therapy: Drugs that attack specific features of cancer cells. Often fewer side effects than chemo.
- Immunotherapy: Treatments that boost the immune system to fight cancer. Side effects may include fatigue and immune reactions.
- Hormonal Therapy: Used for cancers driven by hormones (breast, prostate). It reduces or blocks hormone effects to slow cancer growth.
- Side effects: Any symptom or problem caused by cancer treatment (e.g. pain, nausea, fatigue). Many side effects can be managed with medication or therapy.
- Palliative care: Specialized care focused on symptom relief and quality of life at any stage of illness.
- Clinical trial: A research study of a new treatment or drug. Participation is voluntary and may offer access to new therapies.
- Advance directive: Legal documents stating your medical wishes (e.g. do-not-resuscitate) and appointing a health care proxy if you can’t decide later.
- FMLA: US law guaranteeing eligible workers up to 12 weeks of unpaid, job-protected medical leave for serious health conditions.
All guidance above is based on current cancer care recommendations from authoritative sources (NCI, ACS, CDC, etc.). Each patient’s situation is unique, so use this as a guide and continue to ask your health care team for personalized advice.